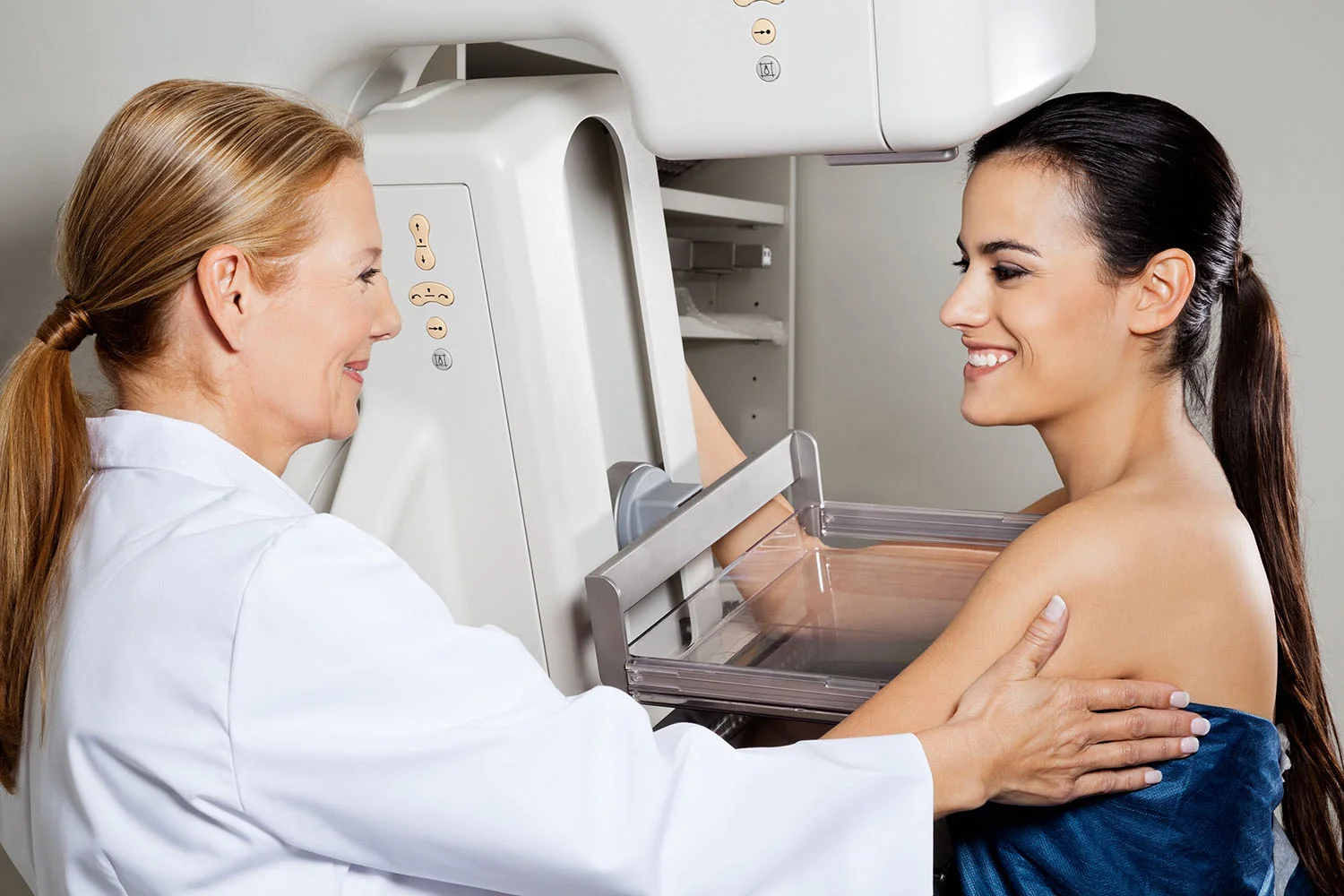
Breast cancer screening guidelines help determine when and how often women should get tested for breast cancer — before any symptoms appear.
Here's a quick summary of the current recommendations from major organizations:
| Organization | When to Start | How Often |
|---|---|---|
| ACS (American Cancer Society) | Age 40 (option); Age 45 (recommended) | Annual (ages 45-54); Every 1-2 years (55+) |
| USPSTF (US Preventive Services Task Force) | Age 40 | Every 2 years (through age 74) |
| ACOG (American College of Obstetricians and Gynecologists) | Age 40 (offer); By age 50 (start) | Every 1-2 years |
| ASBrS (American Society of Breast Surgeons) | Age 40 | Annually |
| High-risk women (BRCA1/2, etc.) | As early as age 25-30 | Annual mammogram + MRI |
These guidelines apply to women at average risk. Women with genetic mutations, dense breasts, or a strong family history may need to start earlier or add supplemental screening.
Breast cancer is the second most common cause of cancer death among women in the US. In 2023 alone, an estimated 43,170 women died from it. But here's the encouraging part: breast cancers found early are smaller, less likely to have spread, and far easier to treat successfully.
That's why knowing your screening schedule — and actually following it — matters so much.
Keeping up with medical recommendations can feel like chasing a moving target. In April 2024, the landscape shifted significantly when the U.S. Preventive Services Task Force (USPSTF) updated its official stance. For years, there was a debate about whether women should start at age 40 or 50. Now, the consensus among major medical bodies is clearer than ever: starting at age 40 saves the most lives.
The USPSTF now recommends that all women begin biennial (every other year) screening at age 40. This shift was prompted by rising breast cancer rates among younger women—incidence in women aged 40 to 49 increased by about 2% annually between 2015 and 2019. By moving the start date up, the Task Force aims to reduce mortality and address the fact that Black women are often diagnosed with more aggressive cancers at younger ages.
Other organizations, like the American Cancer Society (ACS) and the American College of Radiology (ACR), have long advocated for an even more proactive approach. While they agree on the age 40 start, they often recommend annual screenings rather than biennial ones. We believe that regular, consistent imaging is the best way to catch changes when they are most treatable. You can Read the 2024 USPSTF Recommendation Statement to see the full data behind these changes.
Most women fall into the "average risk" category, meaning they do not have a personal history of breast cancer, a strong family history, or a known genetic mutation like BRCA1 or BRCA2. However, being average risk doesn't mean you are at "no risk." In fact, 1 in 8 women in the U.S. will develop breast cancer during their lifetime.
One in six breast cancers occurs in women between the ages of 40 and 49. When we screen this age group, we see a significant reduction in mortality—roughly 15% according to meta-analysis data. For average-risk women, we recommend starting at age 40 with a Mammography exam.
At our center, we use 3D mammography (also called digital breast tomosynthesis) as our standard of care. This technology allows our fellowship-trained radiologists to view the breast in thin "slices," which is much more effective than traditional 2D imaging. It helps us find small cancers that might be hidden by overlapping tissue and significantly reduces the number of "callbacks" or false alarms that cause unnecessary stress.
If you have a known genetic mutation or a significant family history, the standard "average risk" rules don't apply to you. Genetic mutations like BRCA1 and BRCA2 significantly increase the lifetime risk of breast and ovarian cancers. For these women, screening usually starts much earlier—often at age 25 or 30.
High-risk guidelines typically recommend a combination of an annual mammogram and an annual breast MRI. These are usually staggered six months apart so that the breasts are being imaged twice a year. If you aren't sure where you stand, we recommend a formal risk assessment. You can Take the ACS Breast Cancer Risk Assessment to get a better idea of your personal profile.
Our team is here to help you navigate these results. We believe every woman should have a risk assessment by age 25 to 30, especially if there is a history of cancer in the family. This allows us to build a personalized plan before the age when most screenings typically begin.
The "start at 40" rule is now the baseline, but the frequency of screening is where some guidelines differ.
We encourage our patients to participate in shared decision-making with their doctors. This means looking at your personal health history, your breast density, and your own comfort level with risk. For many, the peace of mind that comes with an annual check-up outweighs the slight increase in the chance of a false positive.
Nearly half of all women have "dense" breasts. This simply means there is more glandular and connective tissue than fatty tissue. On a mammogram, both dense tissue and cancer appear white, which can create a "masking effect." It’s like trying to find a white rabbit in a snowstorm.
Starting in September 2024, the FDA requires all mammography centers to notify patients about their breast density. If you have dense breasts, your doctor might recommend supplemental screening to ensure nothing is missed.
If you have been told you have dense tissue, don't worry—it’s very common. It just means we need to be a bit more diligent. You can learn more about our Breast Screening & Diagnosis options to see which supplemental tests might be right for you.
We consider 3D mammography the new gold standard for a reason. Traditional 2D mammograms take pictures from the top and the side, which can result in images where layers of tissue overlap. Digital breast tomosynthesis (3D) takes multiple images from various angles and reconstructs them into a 3D volume.
The benefits of 3D mammography include:
We've invested in this technology because we want the most accurate results for our community. You can read more about why 3D Mammograms: New Standard for Screening is so important for early-stage detection.
One of the most critical reasons for the recent update to breast cancer screening guidelines is the mortality gap affecting Black women. While non-Hispanic White women have the highest incidence of breast cancer, Black women are 40% more likely to die from the disease.
There are several factors at play here:
Starting screening at age 40 is a vital step toward closing this gap, but it isn't enough on its own. We are committed to providing equitable care and ensuring that every woman in Lincoln has access to high-quality imaging and prompt follow-up.
What happens when you reach age 75? Most guidelines, including the USPSTF, state that there isn't enough evidence to recommend for or against screening after this age. However, "age" is just a number; what matters more is your overall health and life expectancy.
The general rule of thumb is to continue screening as long as you are in good health and have a life expectancy of 10 years or more. If you are 78 and active with no major health issues, continuing your annual or biennial mammogram makes sense. If you have significant comorbidities that limit your quality of life, you and your doctor might decide that the harms of screening (like the stress of a biopsy) outweigh the potential benefits.
Most major organizations no longer recommend formal breast self-exams (BSE) because they haven't been shown to reduce mortality and can increase the rate of unnecessary biopsies. However, we strongly advocate for breast awareness. This means knowing how your breasts normally look and feel. If you notice a new lump, skin dimpling, nipple discharge, or persistent pain, you should tell your doctor right away. Most breast cancers in women under 50 are actually self-detected through this kind of awareness.
No medical test is perfect. The "harms" of screening include:
Your doctor can use several validated models to calculate your risk. The Gail Model is commonly used for average-risk women, while the Tyrer-Cuzick Model is often better for those with a strong family history as it takes more detailed genetic information into account. Factors that increase risk include age, family history, early menstruation (before age 12), late menopause (after age 55), and having dense breasts.
Navigating breast cancer screening guidelines shouldn't be a solo journey. Whether you're turning 40 and ready for your first mammogram or you're managing a high-risk family history, we're here for you every step of the way.
AMI is Lincoln’s only ACR Designated Comprehensive Breast Imaging Center. Our fellowship-trained radiologists are sub-specialized in breast health, ensuring you get the most accurate reading possible. Because we are an independent outpatient center, we offer high-quality imaging at outpatient prices—meaning no hospital markups and no surprise bills.
We even offer the AMI Mammo Club and Mammo Party events to make your annual screening a more comfortable, community-focused experience.
Don't wait for symptoms to appear. Early detection is the most powerful tool we have. Request an appointment with our team at our Breast Center today and take control of your health.